The L5 S1 disc is one of the most talked-about structures in spine health, and for good reason. If you or someone you know has experienced lower back pain that radiates into the leg, chances are the L5 S1 Disc is involved. This disc sits at a critical junction of the spine, handling immense pressure and movement every single day.
In this guide, we’ll break down exactly what the L5 S1 disc is, why it’s so vulnerable to injury, how problems develop, and what modern medicine and lifestyle changes can do to manage or even resolve symptoms. Whether you’re dealing with pain, stiffness, or simply want to understand your MRI report better, this article will give you clarity.
Let’s dive deep into the anatomy, symptoms, causes, treatments, and long-term outlook related to the L5 S1 disc.
Understanding the L5 S1 Disc and Its Role in the Spine
The L5 S1 disc is located between the fifth lumbar vertebra (L5) and the first sacral vertebra (S1). This area marks the transition point between the flexible lumbar spine and the rigid sacrum, making it one of the most mechanically stressed regions of the entire spine. Every time you bend, twist, lift, or sit, the absorbs a significant amount of force.
Structurally, the disc is made of two main parts: a tough outer layer called the annulus fibrosus and a softer, gel-like center known as the nucleus pulposus. Together, they function as a shock absorber, preventing bone-on-bone contact while allowing smooth spinal movement. When healthy, the plays a crucial role in maintaining balance, posture, and mobility.
Because this disc supports the upper body’s weight and facilitates motion, it naturally experiences wear and tear over time. This is why the L5 S1 disc is one of the most common sites for disc degeneration, bulges, and herniations, especially in adults over the age of 30.
Common Problems Associated With the L5 S1 Disc
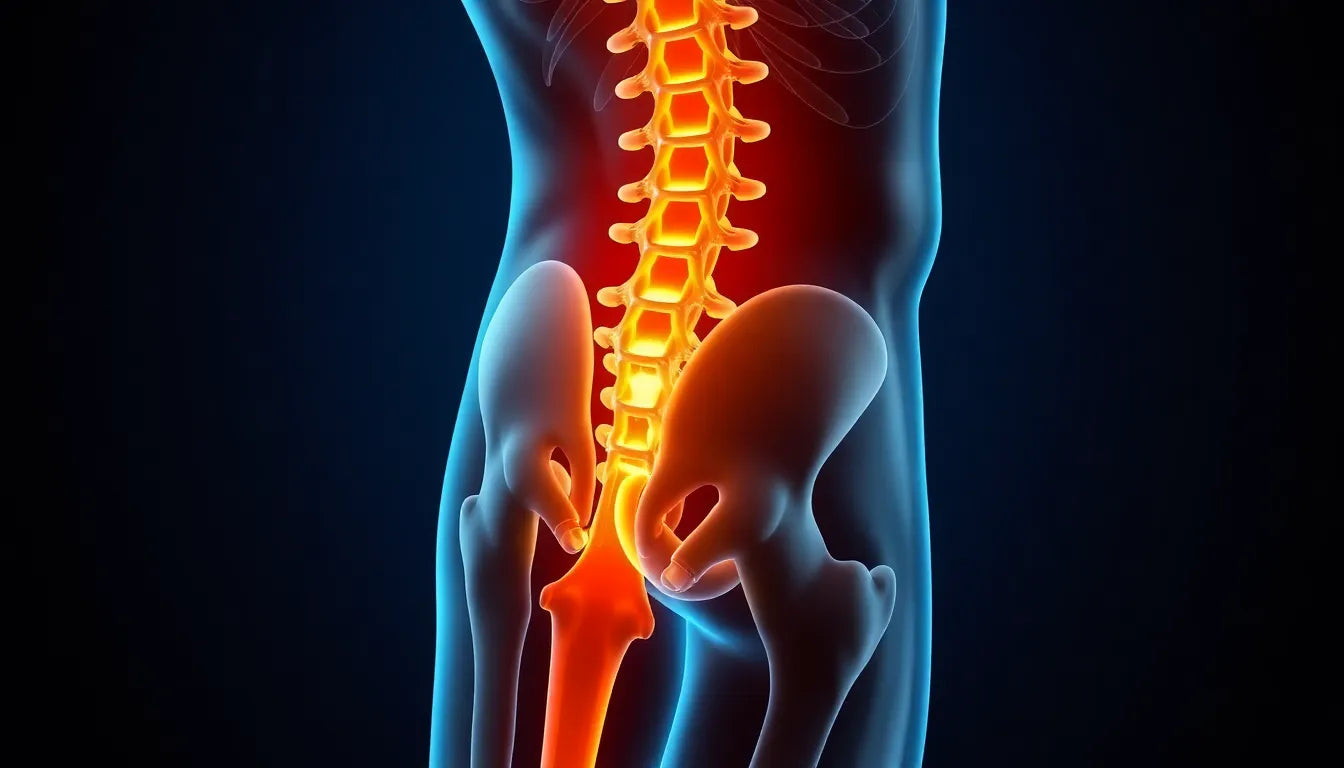
One of the most frequent issues affecting the L5 S1 disc is disc herniation. This occurs when the inner gel pushes through a weakened area of the outer layer, potentially compressing nearby nerves. When this happens at L5 S1, it often affects the sciatic nerve, leading to pain that travels down the leg.
Another common condition is degenerative disc disease, which is not actually a disease but a natural aging process. Over time, the disc loses hydration, becomes thinner, and provides less cushioning. At the L5 S1 level, this degeneration can lead to stiffness, chronic lower back pain, and reduced flexibility.
Disc bulges are also frequently seen at this level. Unlike herniations, bulges involve the disc extending outward without rupturing. While bulges may be painless initially, they can progress and start pressing on nerves, especially if combined with inflammation or spinal narrowing.
Symptoms Linked to L5 S1 Disc Issues
Symptoms related to the L5 S1 disc can vary widely depending on the severity of the problem and whether nerves are involved. Mild disc degeneration may cause nothing more than occasional lower back stiffness, while a herniated disc can trigger intense pain and neurological symptoms.
One of the hallmark symptoms is sciatica, characterized by sharp, burning, or electric-like pain that radiates from the lower back into the buttock, thigh, calf, or foot. This happens because the L5 or S1 nerve roots become irritated or compressed by the damaged disc.
Other common symptoms include numbness, tingling, muscle weakness, and difficulty standing or walking for extended periods. Some people notice pain worsening with sitting, bending forward, or lifting heavy objects, which directly increases pressure on the L5 S1 disc.
Causes and Risk Factors for L5 S1 Disc Damage
Damage to the L5 S1 disc rarely happens overnight. In most cases, it develops gradually due to repetitive stress, poor posture, and lifestyle factors. Sitting for long hours, especially with improper ergonomics, places continuous pressure on this disc and accelerates wear.
Heavy lifting, particularly without proper technique, is another major contributor. Sudden twisting motions while carrying weight can create micro-tears in the disc’s outer layer, making it more vulnerable to bulging or herniation over time.
Genetics also play a role. Some people are born with discs that degenerate faster than average. Combined with factors like smoking, obesity, and lack of physical activity, genetic predisposition can significantly increase the risk of L5 S1 disc problems.
Diagnosis and Imaging of the L5 S1 Disc
Diagnosing an L5 S1 disc problem begins with a detailed medical history and physical examination. Doctors assess posture, range of motion, reflexes, and muscle strength to identify nerve involvement. Simple tests like the straight leg raise can provide valuable clues.
Imaging plays a key role in confirming the diagnosis. MRI scans are considered the gold standard because they clearly show disc structure, nerve compression, and soft tissue changes. MRI reports often mention terms like “L5 S1 disc bulge,” “protrusion,” or “herniation,” which can sound alarming but vary widely in severity.
X-rays may also be used to assess spinal alignment and rule out fractures, though they cannot directly visualize discs. In complex cases, CT scans or nerve conduction studies may be recommended to gain a more comprehensive picture of the problem.
Treatment Options for L5 S1 Disc Conditions
Treatment for issues usually starts with conservative, non-surgical approaches. Rest, activity modification, and physical therapy are often highly effective, especially in the early stages. Targeted exercises help strengthen core muscles, improve flexibility, and reduce pressure on the disc.
Medications such as anti-inflammatory drugs and muscle relaxants may be prescribed to control pain and inflammation. In some cases, epidural steroid injections are used to calm irritated nerves and provide temporary relief, allowing patients to participate more effectively in rehabilitation.
Surgery is considered only when conservative treatments fail or when there is severe nerve compression causing progressive weakness or loss of bladder or bowel control. Procedures like microdiscectomy or spinal fusion can provide excellent outcomes when appropriately indicated, particularly for persistent L5 S1 disc herniations.
Long-Term Outlook and Prevention Strategies
The long-term outlook for L5 S1 disc problems is generally positive, especially with early intervention and proper management. Many people experience significant improvement within weeks to months using non-surgical treatments alone. Even herniated discs can shrink naturally over time as inflammation subsides.
Prevention plays a critical role in maintaining disc health. Maintaining a healthy weight, practicing good posture, and engaging in regular low-impact exercise can dramatically reduce stress on the L5 S1 disc. Core strengthening and flexibility training are particularly beneficial.
Equally important is learning proper body mechanics. Lifting with the legs instead of the back, avoiding prolonged sitting, and taking frequent movement breaks can protect the L5 S1 disc from unnecessary strain. Small daily habits, when practiced consistently, make a big difference in long-term spinal health.
Final Thoughts on the L5 S1 Disc
The L5 S1 disc may be small, but its impact on daily life is enormous. As one of the most commonly affected spinal segments, understanding how it works and why it fails is essential for anyone dealing with lower back pain or sciatica.
The good news is that most problems are manageable and often reversible with the right approach. Modern diagnostics, effective therapies, and lifestyle modifications have made it easier than ever to regain comfort and mobility.
By staying informed, proactive, and consistent with spine-friendly habits, you can protect your L5 S1 disc and maintain a strong, resilient lower back for years to come.